Key Takeaways
- Whooping cough, or pertussis, is a highly contagious respiratory infection that is still prevalent today.
- Cases have been rising in recent years despite longstanding vaccination efforts.
- Outbreaks occur in schools, childcare facilities, hospitals, and communities.
- It’s crucial to recognize symptoms like prolonged cough to get timely diagnosis and treatment.
- Vaccination is vital to reduce spread, along with other precautions like hand hygiene.
- Adults and pregnant women should also get the Tdap booster shot to protect vulnerable infants.
Introduction
Whooping cough, also known as pertussis, is a respiratory illness that has persisted over time despite mass vaccination efforts. The disease is notorious for uncontrollable coughing fits and a “whooping” sound when breathing in. While whooping cough cases had declined for decades after the introduction of vaccines in the 1940s, concerning trends have emerged in recent years. So is whooping cough still around today? Unfortunately, the answer is yes. Understanding why this preventable disease has endured and how to guard against it remains important. This article will provide a comprehensive overview of the continued threat of pertussis, including up-to-date statistics, reasons for ongoing transmission, at-risk groups, prevention strategies, and symptoms requiring prompt medical care. After reviewing the key facts and considerations, readers will have a thorough understanding of this stubbornly persistent infection.
What factors have caused whooping cough cases to rise despite vaccination efforts?
The development of pertussis vaccines in the 1940s led to dramatic reductions in disease rates over subsequent decades. However, within the last 15 years, the number of reported pertussis cases has climbed steadily. For example, the CDC recorded 48,277 cases in 2012 versus just 1,010 in 1976. Several interrelated factors explain why whooping cough has rebounded in the era of mass vaccination:
Is waning immunity among adolescents and adults contributing to pertussis resurgence?
- Yes, waning immunity after vaccination or natural infection appears key. While childhood shots provide protection initially, immunity fades substantially after 5-10 years.
- Many adolescents and adults become vulnerable to contracting and transmitting pertussis again. Research finds their risk increases around 11-15 years post-vaccination.
- When adults get infected, they can unknowingly spread it to infants before severe coughing symptoms emerge.
Are gaps in infant and childhood vaccination also involved?
- Infants are too young for vaccination, relying on herd immunity. But gaps in coverage make that herd protection incomplete.
- Only around 93% of toddlers complete the 4-dose DTaP series. Missing doses or delays leave gaps in protection.
- Areas with more vaccine exemptions also have higher pertussis risk, illustrating the need for widespread community immunity.
Do changes in the bacteria explain increasing pertussis circulation?

- Genetic changes in pertussis bacteria may enhance their ability to spread. New strains emerged after vaccines were introduced.
- Research indicates the strains now causing most disease produce more toxins. They potentially suppress early symptoms, prolonging spread.
- But other factors play a bigger role, since rises occurred in countries using the same vaccine components.
Have improved testing and diagnostics contributed to higher reported cases?
- Wider availability of PCR tests probably enlarged case counts to some degree. PCR detects even asymptomatic pertussis infections.
- Yet evidence shows hospitalizations rose as well. So while better testing contributed, it cannot alone explain the resurgence.
In summary, multiple drivers have enabled pertussis to endure post-vaccine including waning adult immunity, persistent infant susceptibility, pathogen adaptation and more extensive testing. Ongoing vaccination across all age groups remains key to contain further spread.
Where do outbreaks of whooping cough commonly occur?
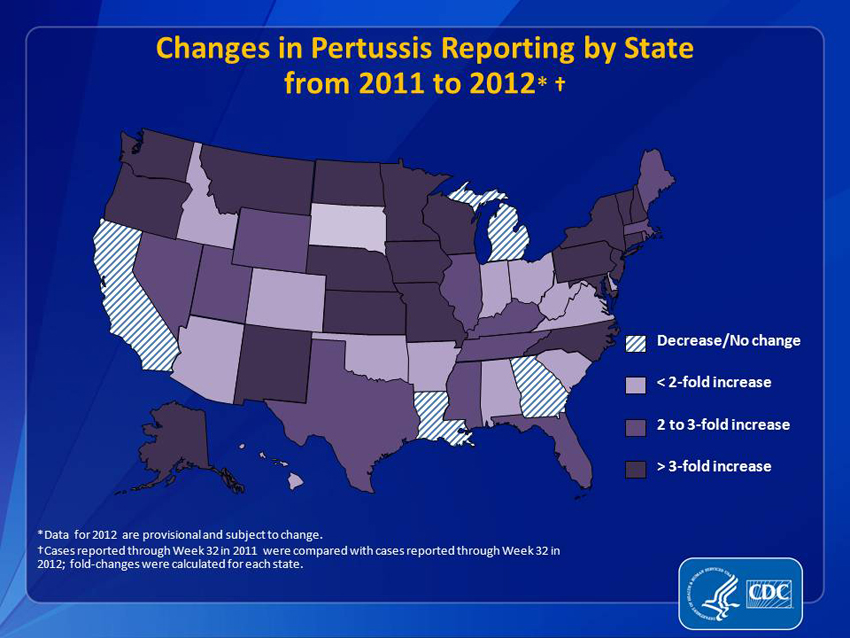
Pertussis outbreaks often emerge in settings where vulnerable individuals frequently interact. Schools, childcare facilities, and healthcare environments are prime locations for transmission. However, sizeable community-wide outbreaks also occur.
Do whooping cough outbreaks happen in schools?
- Yes, school settings are a major site of pertussis spread. Research shows outbreaks most commonly occur in middle and high schools.
- Adolescents in close contact can directly transmit pertussis to one another as their childhood immunity has decreased.
- They may then bring the infection home to younger siblings who are still undergoing vaccination.
Are childcare centers and preschools at high risk for outbreaks?
- Absolutely. Childcare facilities have always faced high rates of pertussis. Infants here are vulnerable if staff or older kids are infected.
- From 1985-1989, an average of 7.5% of U.S. pertussis cases occurred in childcare attendees under 1 year old.
- Childcare centers that require staff Tdap vaccination and enforce exclusion policies during outbreaks see lower transmission.
Can whooping cough spread rapidly in healthcare settings?
- Yes, hospitals and clinics are prime locations for pertussis exposure, especially neonatal and pediatric units.
- Infected healthcare workers can pass pertussis to newborns or unvaccinated children who are extremely susceptible.
- Hospitals with pertussis outbreaks track cases carefully and may temporarily restrict visiting.
How common are wider community-based pertussis outbreaks?
- Wider geographic outbreaks do periodically occur as well. These demonstrate how pertussis can spread broadly when immunity gaps emerge.
- For example, California had a major statewide outbreak in 2014, including over 11,000 cases and hospitalizations.
- Neighborhood, city, or county-wide clusters also occur, like the New York outbreak in 2019 exceeding 200 cases.
In summary, pertussis outbreaks can flare up anywhere susceptible individuals come together, particularly childcare centers, schools, healthcare facilities, and communities displaying rising rates of transmission.
How can parents help prevent whooping cough transmission at home?
Since pertussis spreads so readily between family members in a household, parents must take proactive measures to limit transmission risk at home:
Should pregnant women get the Tdap vaccine?
- Absolutely. The CDC strongly recommends the Tdap vaccine during the third trimester of each pregnancy.
- This maximizes protective antibodies able to cross the placenta to the newborn, guarding against infection in their first months.
- Studies confirm newborns have a lower risk of contracting pertussis if their mother received Tdap while pregnant.
When can infants start getting vaccinated against pertussis?
- The DTaP vaccination series begins at 2 months, with doses at 4, 6, and 15-18 months, plus a 4-6 year booster.
- Getting children vaccinated on schedule closes immunity gaps as soon as possible. Delaying doses raises risk.
Should parents request Tdap boosters for caregivers and relatives?
- It’s wise for close caregivers to get a Tdap booster, especially if a new baby is joining the family.
- Grandparents, relatives providing childcare, and babysitters should check Tdap status with their doctor and get a booster if necessary.
- This “cocooning” strategy walls off vulnerable infants from potential pertussis exposure.
What household precautions help cut transmission risk?
- Avoid close contact and kissing infants if anyone has a cough, fever, or runny nose.
- Wash hands thoroughly after coughing, sneezing, or handling tissues.
- Don’t share eating utensils or drinking cups.
- Disinfect frequently touched surfaces like crib rails, doorknobs, tablets.
By following vaccination guidelines, maintaining hygiene, and restricting contact when ill, families can substantially lower the odds of pertussis infiltrating the home.
How can schools and childcare centers help curb pertussis transmission?
Schools and childcare facilities play a critical role in preventing community-wide pertussis spread. They can take several key steps:
Should childcare staff be required to get Tdap boosters?
- Yes, childcare organizations should mandate that all staff receive a Tdap booster, preferably before starting employment.
- This provides a protective bubble around vulnerable infants who haven’t completed vaccination.
- States like California have enacted laws requiring childcare staff to get Tdap boosters to prevent outbreaks.
When should students be sent home from school during a pertussis outbreak?
- In an outbreak, students with suspected pertussis should be promptly isolated and sent home.
- Most schools mandate students remain home until completing 5 days of antibiotic treatment to become non-infectious.
- Siblings should also be monitored closely for any cough symptoms.
Do schools need to notify parents of pertussis cases?
- Definitely. Clear notification allows parents to monitor children for symptoms vigilantly.
- It also underscores the need for ensuring children’s vaccination status is up to date.
- Confidentiality around infected students should be maintained.
Should childcare programs mandate pertussis vaccines?
- Many experts advise that childcares require enrolled children to be up to date on DTaP shots.
- Those with exemptions could be excluded during outbreak periods to protect vulnerable infants under 12 months old.
- A vaccinated enrollment provides a level of herd immunity surrounding those not yet fully immunized.
Strict control measures in high-risk childcare and school environments are instrumental in disrupting wider community transmission of pertussis.
What are the most common symptoms of pertussis that require medical assessment?
Recognizing the signs and symptoms of pertussis is key to obtaining timely diagnosis and reducing transmission. The hallmark symptom is a persistent cough, often accompanied by:
How does the cough associated with pertussis progress?
- The cough emerges like a mild cold but worsens over 1-2 weeks into severe coughing fits.
- Fits involve repeated bursts of numerous rapid coughs without inhaling, leaving patients gasping for breath, with a “whooping” sound as they inhale.
- Coughing episodes can recur for 6-10 weeks before gradually improving.
- Older children and adults may not have the “whoop” sound so cough duration is important.
Does pertussis cause any other respiratory symptoms?
- Yes, nasal congestion, runny nose, and sneezing are common, similar to a cold early on.
- In infants, apnea – paused breathing – can follow coughing fits.
- Pneumonia is a common complication, causing fever.
When do pertussis complications become more dangerous?
- Infants under 6 months old face the highest risk of life-threatening complications and death.
- Bacterial pneumonia, seizures, brain damage from oxygen loss can occur in severe infant cases.
- Adolescents and adults may lose weight from prolonged coughing and vomiting.
- Coughing can result in bruised ribs, abdominal hernias, or passed out (fainting) spells.
If cough persists longer than a week, especially with “whooping” fits, rapid medical attention is vital to confirm or rule out pertussis through lab testing of nasal secretions. Prompt antibiotic treatment can help minimize complications.
Conclusion
In conclusion, whooping cough remains a persistent public health threat despite long-available vaccines. The disease leads to significant morbidity and mortality, especially in vulnerable infants. Pertussis endures due to waning immunity among older groups, persistent susceptibility in infants, and gaps in vaccine coverage that allow outbreaks to spread, including in childcare, school and healthcare settings. Vigilance around vaccination across all ages, paired with awareness of prolonged cough symptoms, are required to control pertussis. With proper precautions and protection, the threat of this highly contagious respiratory infection can be reduced
- How to Sleep Well with a Broken Arm?
- What Do Urologists Do for Females?
- Are Bulging Veins Dangerous?
- Can You Have Sugar Free Cough Drops with Invisalign?
- What Is Called Antihaemorrhagic Vitamin?
- How to Get Pulse Down to Donate Plasma?
- Why Empaths Can’t Sleep During a Full Moon?
- When Should You Go to the Doctor for a Horse Fly Bite?
- Whats Wrong with April Kepner’s Second Baby?
- Why Has DDT Considered a Good and Effective Insecticide?
- Do They Have Pickleball in Portugal?
- Why Are Dubia Roaches Illegal in Florida?
- Do I Need to Take Medicine on an Empty Stomach or With Food?
- Why Does My PS4 Keep Saying Copying Add On?
- Do Marines Have Brigades?
- Are Opened Clams OK to Eat?
- What Is Bandit Heelers Job?
- How to Become a Company Man in the Oilfield?
- What Is a Counter Statement?
- Why is your Poop Green?
- Are Bats Blind?
- What Does Hydration Percentage Mean?