Key Takeaways:
- During expiration, alveolar pressure becomes greater than atmospheric pressure due to lung recoil.
- The relaxation of the diaphragm and chest wall tissues causes the lungs to deflate.
- Collapsing alveoli increase intra-alveolar pressure to about +1 cmH2O.
- This positive pressure gradient forces air out of the lungs over 2-3 seconds.
- By the end of expiration, alveolar pressure equals atmospheric pressure again.
Introduction
Breathing is an automatic process that involves inhaling oxygen-rich air and exhaling carbon dioxide-rich air. This gas exchange between the lungs and atmosphere enables the body to acquire the oxygen it needs and eliminate waste gases.
But what exactly happens to the pressure inside the air sacs of the lungs during the breathing cycle? More specifically, how does alveolar pressure change during expiration?
This article will provide a comprehensive overview of the pressure dynamics in the alveoli as the lungs exhale. We will evaluate the interplay of key anatomical structures, airway pressures, lung volumes, and other variables that explain the fluctuation in alveolar pressure during expiration.
Gaining an in-depth understanding of this physiological process will shed light on how the respiratory system functions to ventilate the lungs. The analysis will also elucidate how certain lung diseases can disrupt normal alveolar pressure patterns.
- Are Almonds Good for You?
- Is There Room for Negotiation?
- Should Artists Have Total Freedom of Expression?
What Are the Alveoli and What Is Their Role?
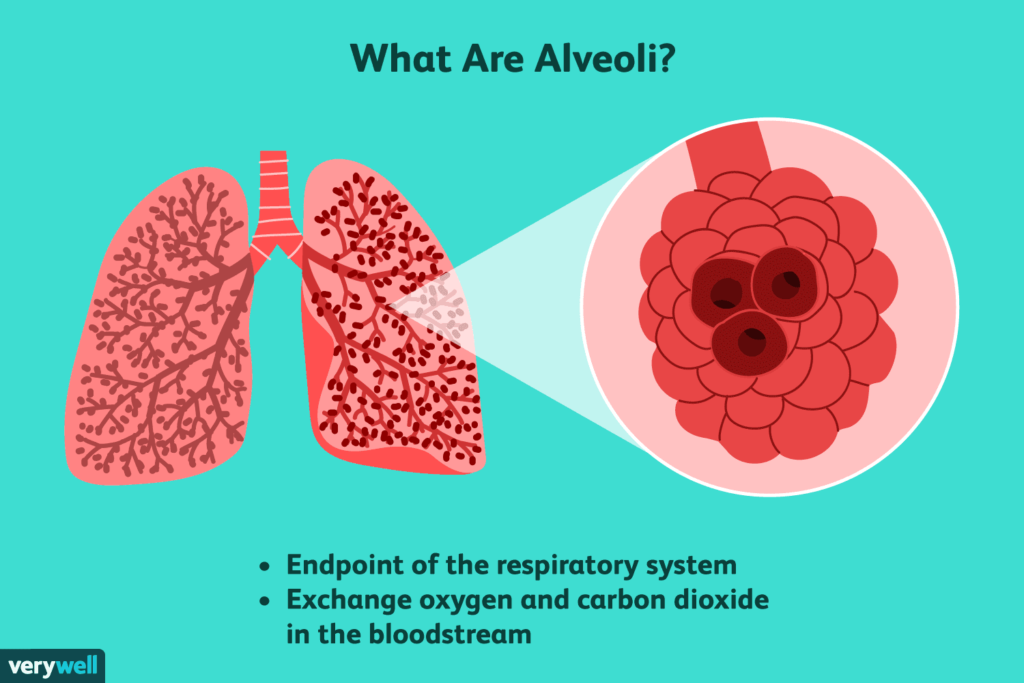
To understand alveolar pressure, we must first briefly review the critical role of alveoli in gas exchange. Alveoli are tiny, elastic air sacs clustered at the ends of the bronchioles in the lungs.
Their walls are extremely thin (just one cell thick), allowing for rapid diffusion of oxygen and carbon dioxide between the air and blood. The lungs contain around 300-500 million alveoli, providing a gigantic surface area of about 70-100 square meters for this gas exchange process, which is known as external respiration.
When you inhale, the alveoli expand as air flows into them. The oxygen passes through the alveolar walls into the pulmonary capillaries, where it binds with hemoglobin in red blood cells. At the same time, carbon dioxide diffuses from the blood into the alveoli to be exhaled.
So the alveoli play a vital role in transferring respiratory gases between the lungs and bloodstream. Now let’s analyze what happens to the pressure inside these tiny air sacs during exhalation.
What Are the Main Factors That Influence Alveolar Pressure During Expiration?
There are three primary factors that impact alveolar pressure as the lungs exhale:
1. Recoil of the Lungs
The lungs and airways are elastic. This means they can stretch when inflated with air during inhalation, then recoil back like a rubber band when air is expelled during exhalation. The lung tissue itself provides an inherent recoil pressure that will cause the lungs to deflate passively.
2. Relaxation of the Diaphragm
The diaphragm is a sheet of muscle that contracts and pulls downward during inhalation to expand the chest cavity volume. When it relaxes during exhalation, the diaphragm moves upward, reducing chest cavity space. This also allows the elastic recoil of the lungs to deflate them.
3. Contraction of the Internal Intercostal Muscles
The intercostal muscles are located between the ribs. The internal intercostals contract during forced exhalation, pulling the rib cage inward, further reducing chest cavity volume to deflate the lungs.
Now that we’ve covered the key factors at play, let’s analyze exactly how alveolar pressure changes during the exhale process.
- Does Elevating Your Legs Help with Circulation?
- How Many Clicks in a 2 mg Ozempic Pen?
- Is Inequality an Equation?
How Does Alveolar Pressure Change During Expiration?
During expiration, alveolar pressure becomes greater than atmospheric pressure as the lungs deflate:
- At the onset of expiration, the alveolar pressure equals atmospheric pressure (about 0 mmHg or 760 mmHg at sea level).
- As exhalation begins, the diaphragm and intercostal muscles relax. The lung tissues elastically recoil while the chest wall springs back outward.
- This decreases the thoracic volume, forcing air out of the alveoli. However, the alveoli first collapse because the airways provide resistance to airflow.
- The collapsing alveoli increase the intra-alveolar pressure to about +1 cmH2O, or approximately +1 mmHg greater than atmospheric pressure.
- This positive pressure gradient drives airflow out of the lungs over 2-3 seconds. Passive deflation accounts for about two-thirds of the exhaled volume.
- By the end of a normal expiration, the alveolar pressure gradually drops back down to equilibrate again with atmospheric pressure (0 mmHg relative to atmosphere).
Therefore, the key events are:
- Lung elastic recoil and diaphragm relaxation reduce thoracic volume.
- Alveoli collapse before air is expelled due to airway resistance.
- Collapsing alveoli raise intra-alveolar pressure to around +1 cmH2O.
- This positive pressure forces about 500 ml of air out of the lungs.
- Alveolar pressure returns to atmospheric levels at the end of expiration.
How Does Alveolar Pressure Differ Between Quiet and Forced Expiration?
So far, we have discussed alveolar pressure changes during a normal, passive expiratory effort, known as quiet expiration. However, we can also forcibly exhale by contracting the internal intercostal muscles.
During a forced expiration:
- More air is exhaled due to added contraction of the intercostals.
- The alveolar pressure increases to higher positive values above atmospheric pressure.
- Exhalation occurs more rapidly over just 1-2 seconds instead of 2-3 seconds.
Therefore, forced expiration further reduces lung volume compared to quiet breathing. This leads to greater collapse of alveoli and higher intra-alveolar pressures to expel air faster and more fully.
- Should a Permitted Occupier Sign a Tenancy Agreement?
- Is Atenolol a Diuretic?
- What Is a Counter Statement?
What Are Some Disease Conditions That Alter Alveolar Pressure During Expiration?
Certain respiratory disorders can disrupt the normal alveolar pressure patterns during exhalation:
- Asthma: Bronchoconstriction increases airway resistance to airflow. This raises intra-alveolar pressures due to greater dynamic lung compression.
- Emphysema: Loss of lung elastic recoil reduces the dynamic compression that helps push air out. As a result, alveolar pressure may not rise sufficiently during exhalation.
- Pulmonary embolism: Blocked blood vessel increases dead space, raising alveolar pressure. Perfusion defects can also decrease carbon dioxide elimination.
- Pneumonia: Inflammation and fluid buildup make alveoli less collapsible, hindering air expulsion. Openings between alveoli may also collapse.
- Pleural effusion: Fluid accumulation in the pleural space increases lung compression. This raises intra-alveolar pressure during exhalation.
- Pneumothorax: Air leak causes lung collapse. The lack of lung recoil can diminish the alveolar pressure increases that normally occur during exhalation.
5 Key Takeaways About Alveolar Pressure During Expiration
- What are the key points to remember about how alveolar pressure changes as air is exhaled from the lungs? Here is a summary:
- Lung elastic recoil and diaphragm relaxation reduce thoracic volume.
- Collapsing alveoli raise intra-alveolar pressure to about +1 cmH2O.
- This positive pressure gradient expels about 500 ml of air over 2-3 seconds.
- Forced expiration increases alveolar pressure further to exhale more air faster.
- Certain lung diseases like asthma can disrupt normal alveolar pressure patterns.
- Is Nickel Plated Steel Magnetic? Unraveling the Complex Science Behind Magnetism
- Why Hyperkalemia Causes Tall T Wave?
- Is Supportful a Real Word?
Conclusion
In summary, the relaxation of the diaphragm and elastic recoil of lung tissue decreases thoracic volume during exhalation. The collapsing alveoli raise intra-alveolar pressure to about +1 cmH2O greater than atmospheric pressure. This positive pressure gradient expels inspired air from the lungs over 2-3 seconds.
By the end of expiration, the alveolar pressure drops gradually back to atmospheric levels. Understanding these dynamics provides insight into the physiology of ventilation and how certain diseases influence alveolar pressure during exhalation
- How Can You Improve Followership Characteristics?
- Does Crying Burn Calories? (Detailed Guide)
- Can you use hydrogen peroxide to clean a bong?
- What’s a Throwaway Statement?
- What Is the Fascinating History of the Bearskin Hat?
- Is There Room for Negotiation?
- Are Bananas Good for You?
- How Does Anthelmintic Resistance Develop?
- Were Added or Was Added?
- Why Are Takis Banned in Canada?
- When Was Stephen Curry Drafted into the NBA?
- Is Atenolol a Diuretic?
- Where Is the Pyramidalis Muscle? An In-Depth Look at this Small Abdominal Muscle
- Is Carpet Powder Safe for Babies? (Explained)
- How to Tell If Someone Turned Their Location off iPhone?
- Are Palm Trees Native to Myrtle Beach? (Myth or True)
- Is Pelli Choopulu Dubbed in Hindi?
- How Many Calories in Jim Beam Peach?
- Can I Wear Invisalign in the Shower?
- How Long Should I Leave Cetaphil on My Face?
- Why Is My Crochet Curving?
- What Is Educators Rising??