Key Takeaways:
- Herpangina is a highly contagious viral illness that causes mouth and throat ulcers.
- It is caused by coxsackieviruses and enteroviruses that spread through contact with respiratory droplets, saliva, mucus, or feces.
- People are most contagious in the first week of infection, even without fever.
- Good hygiene like handwashing and avoiding sharing food or drinks can reduce transmission.
- Antibiotics are ineffective since it is a viral infection, but analgesics help relieve symptoms.
- Does Two Faced Lip Injection Hurt?
- Whats Wrong with April Kepner’s Second Baby?
- Can You Play Flute with Invisalign?
Introduction
Herpangina is a common childhood illness characterized by painful ulcers or sores in the mouth and throat. While herpangina often causes fever along with sore throat, headache, loss of appetite and other flu-like symptoms, fever may be absent in some cases. However, this does not mean the infection is not contagious. In fact, herpangina is highly contagious even without fever.
This article will provide a comprehensive overview of herpangina, its causes, symptoms, contagiousness, and prevention. We will analyze key considerations regarding transmission of the viruses that cause herpangina and explain why it spreads easily regardless of the presence of fever. The depth of information will enable parents to understand this infection and how to reduce its spread.
Recognizing the contagious nature of herpangina is valuable for prompt isolation and hygiene measures. As you read further, you will discover the reasons it tends to affect children, its diagnosis, and the most effective treatment approaches. This will equip you to handle this unpleasant infection and minimize its impact.
What Viruses Cause Herpangina??
Herpangina is caused by viruses in the enterovirus group, primarily coxsackieviruses A and B as well as echovirus and enterovirus 71. These highly contagious viruses spread through contact with respiratory secretions, saliva, feces or other bodily fluids. They can survive on surfaces like doorknobs, toys, utensils etc. for several hours and persist in stool for weeks after infection.
Coxsackievirus A is considered the most common cause of herpangina worldwide. A Taiwan study found that enterovirus 71 caused 74% of herpangina cases during a widespread outbreak in 1998. Other enteroviruses like Coxsackie B and echoviruses are also implicated frequently.
- Are Physiotherapists Doctors in Canada?
- Why Does Skin Lose Elasticity with Age?
- Will a Retracted Eardrum Fix Itself?
How Does Herpangina Spread So Easily??
The tiny enteroviruses that cause herpangina spread through direct contact with virus-laden secretions of an infected person. When the infected individual coughs or sneezes without covering their mouth, they expel tiny droplets containing the virus into the air which can immediately infect anyone nearby.
These respiratory droplets containing virus can also survive on surfaces for hours. If another child puts their fingers in their mouth after touching the contaminated surface, they can get infected. Furthermore, the viruses remain present in the stool for 6-8 weeks even after the infection resolves. Any indirect fecal-oral transmission via contaminated food or surfaces could spread infection.
Since the viruses thrive and multiply in the throat and mouth, saliva is the most contagious source. Sharing food, drinks, utensils, toys or kissing with someone who has herpangina greatly increases the risk of catching the infection. This is why herpangina tends to rapidly spread in childcare centers and schools.
Why Is Herpangina Contagious Without Fever?
Herpangina causes fever in the majority of cases, along with sore throat and mouth ulcers. However, some children develop all the mouth and throat symptoms without much fever. How can herpangina be contagious even without a significant fever?
The incubation period of herpangina is 3-6 days. This means the person is infected and contagious for 3-6 days before onset of noticeable symptoms. Even before ulcers develop in the throat, the viruses multiply and shed from the throat and feces.
Additionally, some children may have a milder illness without high fever due to factors like prior immunization, partial immunity or host genetics. But their oral secretions still teem with viruses that can readily infect others. Hence herpangina transmission from an infected child is not dependent on or related to the presence of fever.
- Can You Play Clarinet with Invisalign?
- How to Read a Ddc Paternity Test Result?
- When Does Foreshortening Occur?
Why Does Herpangina Mostly Affect Children?
While herpangina can occur in adults, it is overwhelmingly a disease of children, especially those under 10 years old. What factors account for this age-related pattern?
Firstly, children have lower immunity to the implicated viruses and are encountering them for the first time. Secondly, younger children have hygiene habits like thumb-sucking or mouthing toys that facilitate transmission. Close interaction with other children further enables spread.
The mouth ulcers in herpangina are most painful between 4-6 years of age due to the prominent papillae on the tongue surface. By adulthood, most individuals develop enough antibodies through prior exposure to be immune to further infection. However, adults with reduced immunity or in contact with infected children may still contract herpangina.
How Is Herpangina Diagnosed?
Healthcare providers can often diagnose herpangina based on the characteristic symptoms of oral ulcers concentrated on the soft palate, tonsils and back of throat along with sore throat and difficulty swallowing. Testing involves taking a throat swab to confirm the presence of enterovirus by viral culture or polymerase chain reaction (PCR) methods.
Blood tests show elevated white cell counts indicating infection. It may be necessary to exclude other causes like strep throat, Hand-Foot-Mouth disease or oral thrush based on swab results. The painful ulcers last for 7-10 days and resolved without scarring.
- When Does an Unfilled Prescription Expire?
- What Blood Type Is the Universal Donor?
- What Is the Survival Rate for Turner Syndrome?
What Is the Incubation Period for Herpangina?
The incubation period of herpangina is typically 3 to 6 days between the time of exposure to an infected person and onset of symptoms. During this incubation phase, the viruses multiply and spread before the immune system responds with fever and inflammation.
The incubation period for coxsackievirus can be as brief as 2 days or as long as 10 days. For enterovirus 71, it ranges from 3 to 7 days. During this phase, the infected person can unknowingly transmit the infection to others. Isolation should begin immediately once ulcers appear to prevent further contagious spread.
Is Herpangina Contagious After the Fever Goes Away?
The fever in herpangina may resolve after the first 2-3 days of illness while the oral ulcers take 7-10 days to heal completely. Does this mean the infection is no longer contagious once the fever goes away?
Unfortunately, children remain contagious for the entire duration of oral ulcer symptoms even after the fever has resolved. The viruses continue to shed and replicate in the throat and stools over the ulcerative phase. So contact with saliva and stools continues to pose an infection risk until the ulcers disappear.
To prevent transmission to others, children should avoid school and minimize contact until all their mouth ulcers have healed. Good hygiene practices should be followed carefully during this period.
- Forefoot, midfoot or heel: How do you walk correctly? 
- Why Are Crystalloids Used in Sepsis?
- Why Exercise Is Important?
How Long Is Herpangina Contagious?
Herpangina is highly contagious from 3 days before the ulcers appear till at least 1 week after the onset of oral ulcers. The peak contagious period is during the first 3-5 days of symptomatic illness when viral shedding from the throat is very high.
Some individuals, known as carriers, continue to shed virus for up to 6 weeks even after ulcers heal while showing no symptoms themselves. This highlights the need for meticulous hand hygiene in outbreak settings to limit further spread from such carriers.
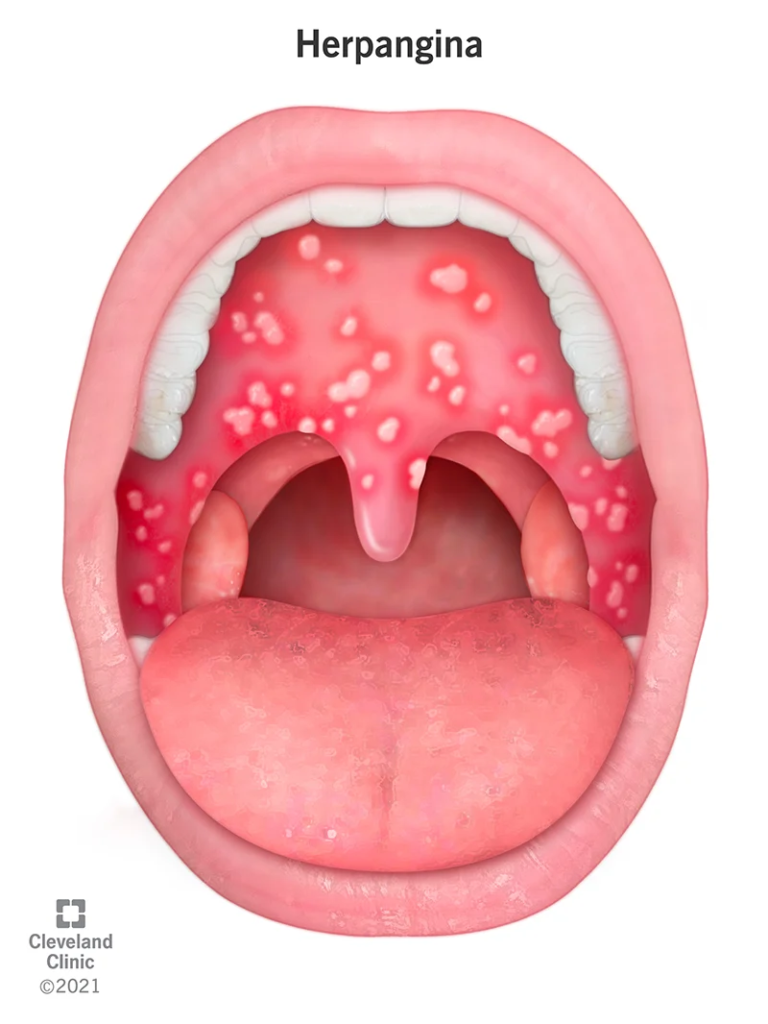
What Are the Symptoms of Herpangina?
The most distinctive symptoms of herpangina are multiple painful ulcers or blisters on the:
- Tonsils
- Back of the throat
- Soft palate
- Uvula
Additional symptoms include:
- Sore throat
- Fever
- Enlarged neck lymph nodes
- Loss of appetite
- Difficulty swallowing
- Headache
- Nausea or vomiting
- General malaise
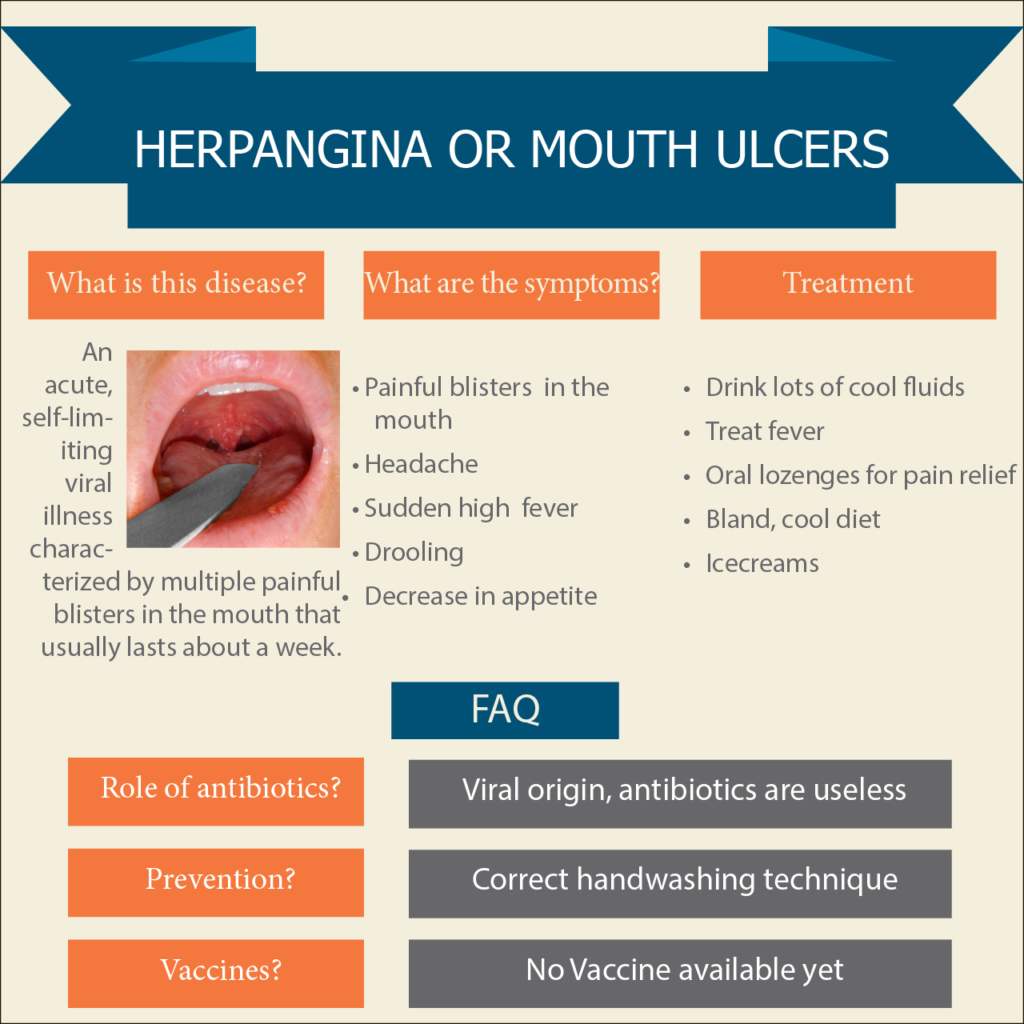
Younger children may complain of stomach ache instead of sore throat pain. They tend to refuse food and drinks due to throat pain, putting them at risk for dehydration.
- How to Make a Split Level Home Handicap Accessible?
- Does Coffee Cause Acne? (Detailed Guide)
- How to Sleep Well with a Broken Arm?
How to Prevent Spreading Herpangina?
Preventing the spread of herpangina requires isolating the infected child and practicing excellent hygiene:
- Keep the child home from school/daycare until ulcers resolve.
- Wash hands frequently with soap and water, especially after touching throat secretions or using the toilet.
- Avoid sharing food, drinks, utensils, toys or personal items.
- Cover mouth and nose when coughing or sneezing.
- Disinfect surfaces like doorknobs, counters, toys.
- Avoid kissing on the lips.
- Wash soiled clothes, bedding and towels with hot water and detergent.
- Avoid exposure to others with weakened immunity.
- Breastfeeding can continue as it provides antibodies to the child.
Are Antibiotics Effective Against Herpangina?
Since herpangina is caused by viruses, antibiotics like penicillin are not effective. They may be prescribed if a secondary bacterial infection occurs. Antibiotics are also ineffective for viral pharyngitis, tonsillitis and most common colds and flu.
However, analgesics like acetaminophen or ibuprofen can relieve sore throat and fever. Plenty of fluids and cold foods like ice cream or popsicles help soothe throat pain. Most cases resolve within 7-10 days without specific treatment.
- What Is a Mental Breakdown?
- Can You Play Clarinet with Invisalign?
- What Are Some Symptoms of the New Omicron Variant of COVID-19?
Can Herpangina Lead to Complications?
In most healthy children, herpangina follows a benign course and resolves without complications within 10 days. Excellent hygiene and isolating infected children limits its spread. But infants, immunocompromised individuals and those with underlying illness are at risk of complications like:
- Dehydration from poor oral intake and vomiting
- Encephalitis (brain inflammation)
- Meningitis (swelling of brain/spinal cord membranes)
- Facial nerve paralysis
- Heart and lung infections
- Sepsis
Enterovirus 71 specifically can rarely cause neurological complications like brainstem encephalitis. Seek urgent care if high fever persists beyond 2 days or the child develops neurological symptoms.
How is Herpangina Different from Hand, Foot and Mouth Disease?
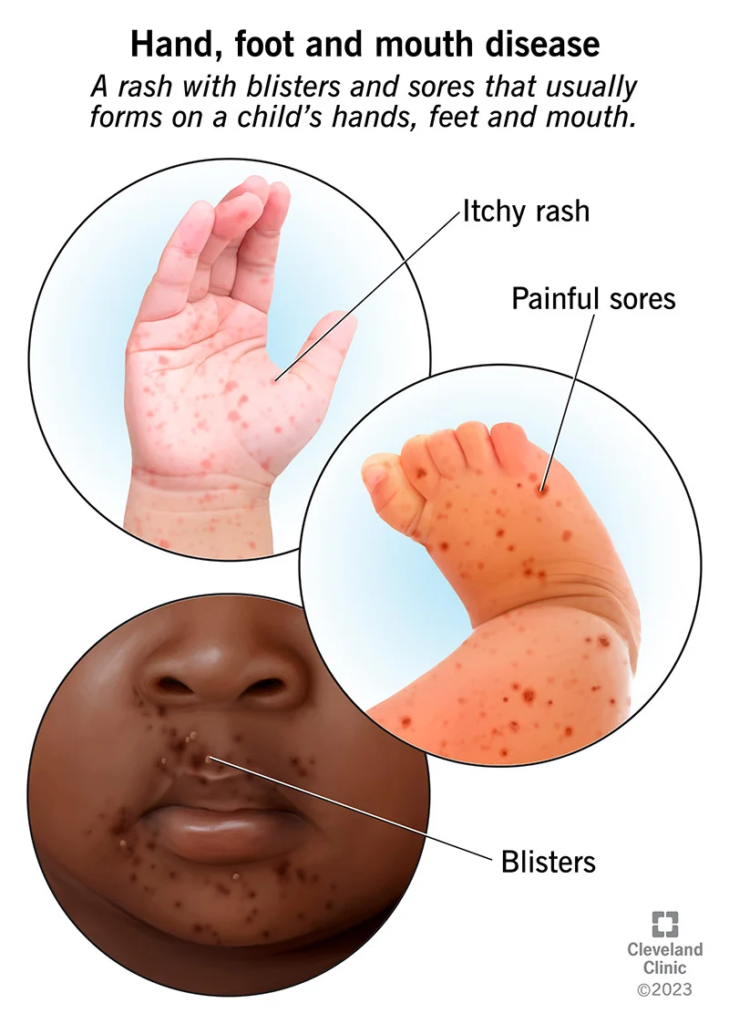
Hand, foot and mouth disease (HFMD) is often confused with herpangina as both cause oral ulcers and sore throat. However, they differ in the following aspects:
- Causes: HFMD is caused by coxsackievirus A16 while herpangina involves coxsackie B and other enteroviruses.
- Rash: HFMD causes a vesicular rash on the palms, soles and buttocks, which is absent in herpangina.
- Ulcers: The ulcers in HFMD are on the tongue, gums and inner cheeks while herpangina ulcers affect the back of the throat.
- Age: HFMD commonly affects those under 5 years old while herpangina primarily affects children over 3 years of age.
- Seasonality: Herpangina peaks in summer and fall while HFMD occurs more in spring and early summer.
- Severity: Herpangina ulcers are often more painful than HFMD.
Can Adults Get Herpangina?
Herpangina most commonly affects children under 10 years old. However, adults can also develop herpangina through contact with infected children. Those at highest risk include:
- Parents or family members of infected children
- School teachers
- Healthcare workers
- Caregivers in daycare centers or pediatric wards
- Those working with children like coaches
- Military recruits in semi-closed settings
- Immunocompromised adults
- Pregnant women
- Adults with heart or lung disease
Any adult exposed to the saliva, nasal discharge or feces of infected children may get herpangina, though symptoms are typically milder. Strict handwashing when handling children with herpangina reduces this risk.
Can You Get Herpangina Twice?
The viruses that cause herpangina do not provide long-lasting immunity. It is possible to develop herpangina more than once in a lifetime. However, second or subsequent infections tend to be less severe due to some retained immune defenses against the virus.
Young children are at greatest risk of recurrent infection since their immunity is not well-developed. Older children and adults are less prone to reinfection but it can still occur occasionally depending on the particular virus. Vaccines are currently unavailable for the viruses implicated in herpangina.
- Does Crying Burn Calories? (A Comprehensive Evaluation)
- Does Spicy Food Help with Sickness?
- Does Two Faced Lip Injection Hurt?
How to Care for a Child With Herpangina
Caring for a child with herpangina involves the following measures:
- Give acetaminophen or ibuprofen for fever and throat pain.
- Offer cold, soft foods like ice cream, popsicles and jello. Avoid acidic or spicy food.
- Encourage fluid intake and watch for dehydration. Offer small frequent sips of water.
- Prevent choking or vomiting by ensuring the child is upright during feeds.
- Use a cool-mist humidifier to moisturize sore throat.
- Salt water gargles provide temporary pain relief for older children.
- Ensure proper rest and keep the child quiet and calm.
- Monitor for high fever lasting over 2 days or other concerning symptoms.
With supportive care, herpangina usually resolves without complications within 7-10 days. Call your pediatrician if the child is unable to swallow saliva or if symptoms worsen or persist longer.
Conclusion
Herpangina is a highly contagious viral infection marked by oral ulcers that afflicts children worldwide. Even without significant fever, children remain contagious for the entire duration of throat ulcer symptoms. Meticulous hygiene and avoiding contact with infected children limits spread of infection. While uncomfortable, herpangina follows a self-limited course in otherwise healthy children with supportive treatment. Understand its contagious patterns, recognize symptoms early and take preventive steps to keep the infection under control.
- Which Immunoglobulin Is Present in Breast Milk?
- Does Coffee Help in Weight Loss??
- Can You Have Cough Drops with Invisalign?
- Are Shingles Contagious?
- Is Sun Gazing Harmful to Your Eyes??
- When Does an Unfilled Prescription Expire?
- How to Make a Split Level Home Handicap Accessible?
- Are Epidermoid Cysts Painful?
- What Is the Ramsay Hunt Syndrome? [Symptoms, Causes, Treatment]?
- Why Are NFTs Bad for the Environment?
- Who Practices Polygamy in the United States?
- How to Change Ford F150 from KM to Miles?
- How Did Dan Fogelberg Meet His Wife?
- Do Twins Count As Para 2?
- Are AirPods Waterproof?
- Will a Cortisone Shot Help a Torn Hip Labrum?
- Can I see who views my collections on Facebook?
- What Is Saifi Saidi Caidi?
- Are Canned Yams Already Cooked?
- Is Rimuru Stronger Than Clayman?