Key Takeaways
- Osteitis pubis causes pain in the groin and lower abdomen, at the pubic symphysis joint.
- The main symptom is a constant dull ache or throbbing pain when moving.
- Pain can also radiate down the inner thighs from the groin area.
- Patients often have anterior and medial groin pain or lower abdominal pain.
- Understanding the pain patterns can aid diagnosis and treatment.
- Which Books Are in Dickensian?
- Are the Sides of a Right Angled Triangle Equal?
- What Does “Elusiveness” Mean in Literature??
Introduction
Groin and pelvic pain can originate from a variety of sources, making it difficult to pinpoint the exact cause. One potential source of chronic groin and lower abdominal discomfort is a condition known as osteitis pubis. This inflammatory condition specifically affects the pubic symphysis joint and surrounding musculoskeletal structures. Given the complex nature of pelvic and groin anatomy, identifying the precise location and patterns of osteitis pubis pain provides useful diagnostic clues. This comprehensive article will analyze in detail the typical sites and characteristics of osteitis pubis pain.
Understanding where patients hurt is the first step toward accurate diagnosis and effective treatment. By evaluating the specific pain profile associated with osteitis pubis, readers will gain valuable insights into assessing and managing this debilitating condition. The content draws on scientific research and clinical expertise to map the pain patterns in an accessible way. Read on to learn all about where osteitis pubis pain manifests.
Where Does Osteitis Pubis Cause Pain?
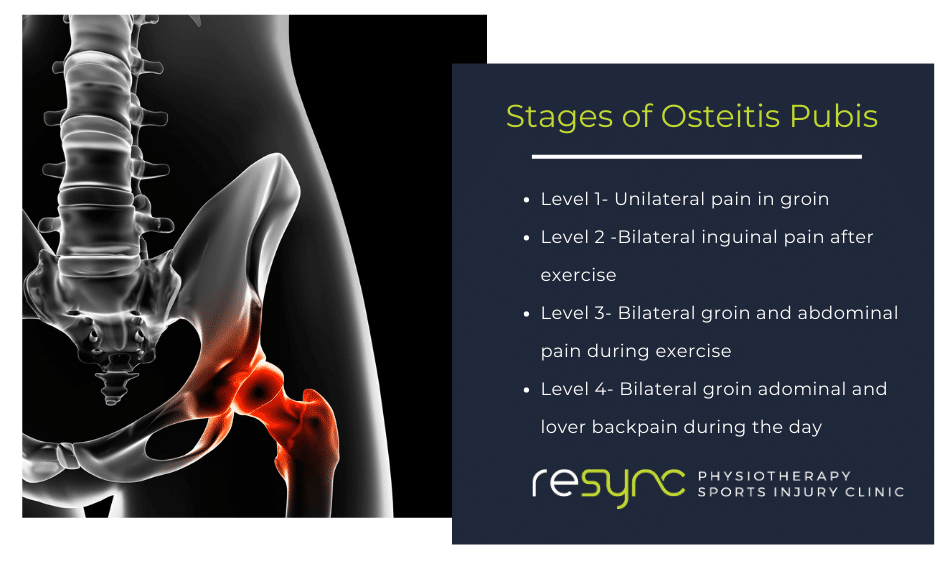
Osteitis pubis refers to inflammation within the pubic symphysis joint, which is located between the left and right pubic bones in the front of the pelvis. This joint is stabilized by a network of ligaments and muscle attachments. Osteitis pubis disrupts the stability of the joint, leading to pain and loss of function. But where exactly does this type of pain present?
Anterior Groin Pain
The most common site of pain with osteitis pubis is in the anterior groin region. Patients often describe an aching or throbbing sensation directly over the pubic symphysis joint. This anterior groin pain tends to be symmetrical on both sides of the midline. It is typically exacerbated by movements that increase stress across the joint, like walking, running, pivoting, kicking, and hip flexion or adduction. A constant dull ache in the anterior groin is a hallmark of osteitis pubis.
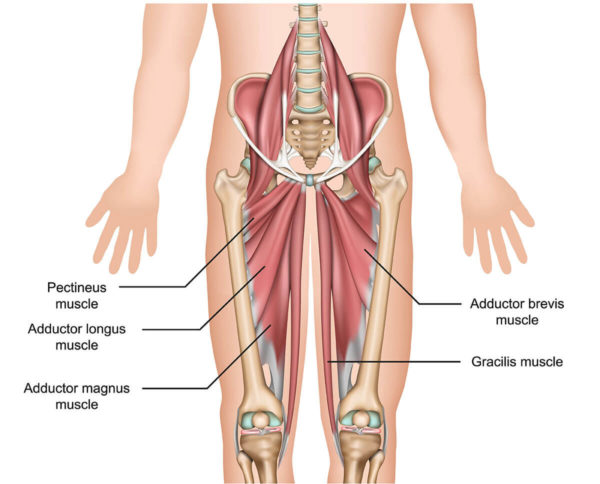
Medial Groin Pain
In addition to anterior groin discomfort, patients commonly report pain along the medial groin area as well. This includes the inner thighs adjacent to the genitals. Medial groin pain may be due to irritation of the adductor muscles that attach near the pubic symphysis joint. The adductors help squeeze the legs together, so actions like striding, twisting, and pivoting can provoke medial groin pain related to osteitis pubis inflammation.
Lower Abdominal Pain
Some individuals with osteitis pubis also experience pain in the lower abdomen below the navel. This occurs because the lower abdominal muscles attach across the front of the pelvis near the pubic symphysis. The abdominal muscles contract forcefully during sit-ups, coughing, or any movement involving the trunk. This can translate tugging forces across an already irritated pubic joint. Lower abdominal soreness may even precede overt groin pain in some osteitis pubis cases.
Inner Thigh Pain
In advanced stages, osteitis pubis pain can radiate down the upper inner thighs as well. The adductor muscles that attach near the pubic symphysis joint originate along the length of the thigh bones. Inflammation and dysfunction at the pubic joint may cause a secondary pain response within the proximal adductor muscles. Patients may feel a dull ache or tightness down the inside of the thighs.
Perineal or Testicular Pain
Less common symptoms include perineal discomfort between the anus and genitals or testicular pain. Some ligamentous supports of the pubic symphysis extend toward perineal structures. Additionally, branches of the same spinal nerve roots supply sensation to both the groin and perineal areas. Referred pain into these regions implies severe instability and inflammation of the pubic joint.
- WHAT HAPPENS IF THE OTHER DRIVER WAS UNINSURED?
- How Is Europium Extracted?
- What Does “Admit Impediments” Mean? Unpacking the Meaning of This Phrase in Shakespeare’s Sonnet 116
Characteristics of Osteitis Pubis Pain
In addition to pinpointing the location of pain, it is also important to understand the typical characteristics and patterns associated with osteitis pubis:
- Constant Ache – Patients often describe a constant, dull ache or feeling of pressure over the pubic area rather than severe, sharp pain. This distinguishes osteitis pubis from acute muscle strains.
- Activity-Related Pain – Symptoms are exacerbated by movements and actions that stress the pubic joint, like running, kicking, squatting, or hip adduction. Relief comes with rest.
- Insidious Onset – Gradual onset of groin pain over days to weeks is typical, rather than sudden acute injury.
- Variable Radiation – Pain may stay localized to the anterior groin or radiate to the abdomen, medial thighs, or perineum depending on severity.
- Morning Stiffness – Stiffness and ache over the pubic symphysis after getting out of bed that improves with activity is characteristic.
- Mechanical Symptoms – Clicking, popping, or grinding sensations may occur with hip/pelvic movements.
Paying attention to these patterns helps distinguish osteitis pubis pain from other causes like hip arthritis, hernias, prostate issues, etc.
Why Does Osteitis Pubis Cause Pain in These Areas?
To understand why osteitis pubis manifests pain in the characteristic distribution, it helps to examine the anatomy and function of the pubic symphysis joint:
- The pubic bones meet at a cartilaginous disc that allows slight motion of the pelvis.
- Powerful ligaments reinforce the joint anteriorly, posteriorly, and inferiorly.
- Several muscles attach near the joint, including the rectus abdominis, adductors, abdominals, and hip flexors.
- These muscles contract forcefully to facilitate running, kicking, twisting, coughing and other strenuous actions.
- Inflammation of the pubic joint and surrounding ligaments reduces joint stability.
- Muscle attachments are irritated with repetitive force transmission across the joint.
- This collective instability and inflammation provokes pain in the groin, lower abdomen, medial thighs, and sometimes perineum.
- Referred pain patterns follow the distribution of underlying neurological innervation.
Therefore, the characteristic location of osteitis pubis pain directly reflects the anatomical structures affected.
- Is Anemia a Prefix?
- Are Daddy Long Legs Spiders?
- What Is the Harmonised Master List of Infrastructure?
Diagnosing Osteitis Pubis Based on Pain Patterns
The location and quality of pain provide clues to differentiate osteitis pubis from other diagnoses. Here are some key patterns in osteitis pubis pain that can aid diagnosis:
- Bilateral groin pain, unlike unilateral pain from a muscle strain or hip disorder.
- Pubic point tenderness, rather than joint line hip pain suggestive of arthritis.
- Absence of abdominal wall pain on palpation, which would indicate a strain or hernia instead.
- Exacerbation by adduction and abdominal activation, indicative of pubic joint irritation.
- Lack of vaginal, urethral or testicular pain that would imply a disorder of those pelvic organs.
- Normal urinalysis findings without infectious symptoms of urine or prostate.
- Hip range of motion within normal limits, rather than limited by joint arthritis.
Together with imaging and physical exam, the pain profile can confirm a diagnosis of osteitis pubis.
How Is Osteitis Pubis Pain Treated?
Once osteitis pubis is diagnosed, management focuses on relieving pain, promoting healing of inflamed structures, and stabilizing the pelvis. Common treatments include:
- Rest from aggravating athletic activities to allow the pubic symphysis to heal.
- Physical therapy to improve flexibility, strength and pelvic stability.
- Anti-inflammatory medications like NSAIDs to control pain and swelling.
- Pubic bone strapping to compress and stabilize the joint.
- Steroid injections into the pubic joint space to directly reduce inflammation.
- Surgery only if conservative measures fail, to shave irritated cartilage or fuse the joint.
With appropriate treatment guided by a clear understanding of the pain profile, most cases of osteitis pubis can resolve within 6-12 weeks.
Conclusion
In summary, osteitis pubis pain most prominently affects the anterior groin region directly over the pubic symphysis joint. Additional pain sites include the medial groin, lower abdomen, inner thighs and sometimes perineum. This reflects the underlying musculoskeletal structures impacted. Recognizing the distinct pain patterns is key for accurate diagnosis. By precisely localizing and characterizing the pain, practitioners can better evaluate and treat osteitis pubis to reduce disability from this debilitating condition
- Where Are Bootstrap Glyphicons Stored?
- Which Immunoglobulin Is Present in Breast Milk?
- Did Lapu Lapu Fight Magellan?
- How to Make Positrons?
- What Is Shear Plane Definition?
- Where Does Applied Science Take You?
- What’s a Throwaway Statement?
- Is Phosphate a Polyatomic Ion?
- Does Deferred Adjudication Show Up on Your Record?
- Should Artists Have Total Freedom of Expression?
- What Does the Wrench Light Mean on a Ford F150?
- How to Make a Gantt Chart in Keynote?
- What Do Yeti Numbers Mean?
- How to Start a Teeth Whitening Business?
- How to Change Input on Samsung Hospital TV?
- where does pickleball central ship from?
- Can you get Mario Kart on Xbox?
- Are Derivations Important for NEET?
- What’s the Difference Between Yamaha FZ and MT?
- Why Do Prices Go Up Faster than Inflation?
- How Much Does It Cost to Install Nema 14 50?
- Does Time Machine Backup Everything on Your Mac?